As providers, how we refer to patients — in written and more commonly, verbal clinical communication — is often biased or stigmatizing.
This can impact clinical care in unanticipated ways.
Some highlights from our workshop on reframing these tendencies https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">
A brief https://abs.twimg.com/emoji/v2/... draggable="false" alt="🧵" title="Thread" aria-label="Emoji: Thread"> 1/x https://twitter.com/MedEdPORTAL/status/1366811842882854912">https://twitter.com/MedEdPORT...
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🧵" title="Thread" aria-label="Emoji: Thread"> 1/x https://twitter.com/MedEdPORTAL/status/1366811842882854912">https://twitter.com/MedEdPORT...
This can impact clinical care in unanticipated ways.
Some highlights from our workshop on reframing these tendencies
A brief
How do we define stigmatizing, biased clinical language?
- Casting undue doubt: "claims he has 10/10 pain"
- Implying undue culpability
- Perpetuating stereotypes
- Including details that are unnecessary to care and might bias future providers: e.g., criminal history
2/x
- Casting undue doubt: "claims he has 10/10 pain"
- Implying undue culpability
- Perpetuating stereotypes
- Including details that are unnecessary to care and might bias future providers: e.g., criminal history
2/x
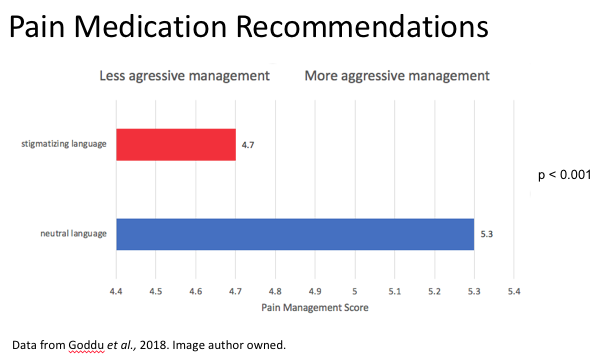
Some examples of neutral language (blue), as compared to stigmatizing or biased language (red), in describing a patient with sickle cell disease presenting to the ED with a vaso-occlusive crisis
https://bit.ly/2Ps4dQy ">https://bit.ly/2Ps4dQy&q...
3/x
https://bit.ly/2Ps4dQy ">https://bit.ly/2Ps4dQy&q...
3/x
The use of biased clinical language was associated with less aggressive treatment of pain associated with a hypothetical patient& #39;s sickle cell vaso-occlusive crisis  https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">
https://bit.ly/2Ps4dQy ">https://bit.ly/2Ps4dQy&q...
4/x
https://bit.ly/2Ps4dQy ">https://bit.ly/2Ps4dQy&q...
4/x
Conditions associated with chronic pain often fall in the category of "medically inexplicable" or contested illnesses — and ones that more often affect women
Clinical language often emphasizes the absence of “objective” or “organic” causes, rather than legitimizing symptoms
5/x
Clinical language often emphasizes the absence of “objective” or “organic” causes, rather than legitimizing symptoms
5/x
Gender norms around pain perception and expression, combined with the fact that these conditions are under-researched, lead to these descriptors.
Overall, this clinical language leads to men’s pain being more readily believed and treated.
https://bit.ly/3sL3mca ">https://bit.ly/3sL3mca&q...
6/x
Overall, this clinical language leads to men’s pain being more readily believed and treated.
https://bit.ly/3sL3mca ">https://bit.ly/3sL3mca&q...
6/x
We suggest these reflective questions to guide clinical documentation that is free of bias and stigma  https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">
7/x
7/x
Ask these questions and assess baseline assumptions as you frame clinical documentation to ensure it& #39;s free of bias and stigma
8/x
8/x
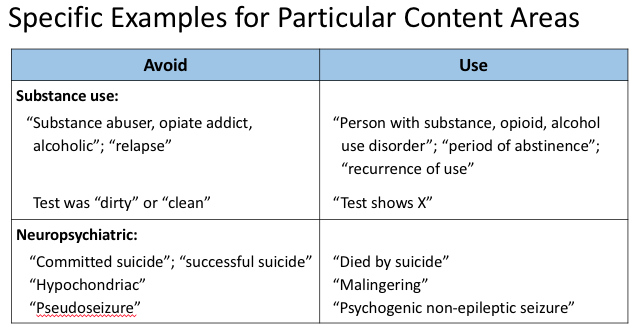
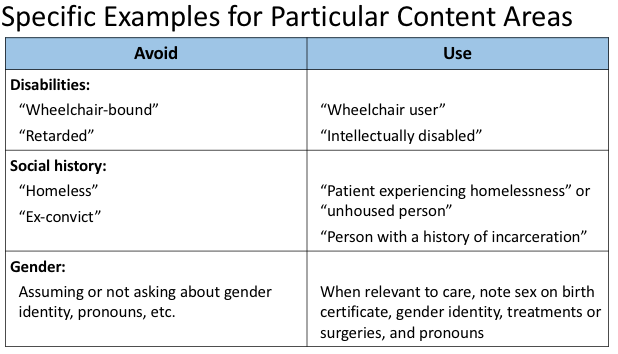
Some special considerations for clinical language as they apply to:
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">substance use disorder
https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">substance use disorder
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditions
https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditions
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilities
https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilities
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social history
https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social history
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity
https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity
9/9
Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi
9/9
Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi
Adding our non-Twitter-dwelling co-conspirators: Tiffany Lee, MD, Samuel Ricardo Saenz, MD, MPH, Peter Leahy, MD, Carrie Johnson, MBA, Cynthia Kapphahn, MD, MPH

 Read on Twitter
Read on Twitter


 https://bit.ly/2Ps4dQy&q... 4/x" title="The use of biased clinical language was associated with less aggressive treatment of pain associated with a hypothetical patient& #39;s sickle cell vaso-occlusive crisis https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)"> https://bit.ly/2Ps4dQy&q... 4/x" class="img-responsive" style="max-width:100%;"/>
https://bit.ly/2Ps4dQy&q... 4/x" title="The use of biased clinical language was associated with less aggressive treatment of pain associated with a hypothetical patient& #39;s sickle cell vaso-occlusive crisis https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)"> https://bit.ly/2Ps4dQy&q... 4/x" class="img-responsive" style="max-width:100%;"/>


 7/x" title="We suggest these reflective questions to guide clinical documentation that is free of bias and stigma https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">7/x" class="img-responsive" style="max-width:100%;"/>
7/x" title="We suggest these reflective questions to guide clinical documentation that is free of bias and stigma https://abs.twimg.com/emoji/v2/... draggable="false" alt="👇🏾" title="Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)" aria-label="Emoji: Rückhand Zeigefinger nach unten (durchschnittlich dunkler Hautton)">7/x" class="img-responsive" style="max-width:100%;"/>

 substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi" title="Some special considerations for clinical language as they apply to:https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi">
substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi" title="Some special considerations for clinical language as they apply to:https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi">
 substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi" title="Some special considerations for clinical language as they apply to:https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi">
substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi" title="Some special considerations for clinical language as they apply to:https://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">substance use disorderhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">other neuropsychiatric conditionshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">disabilitieshttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">social historyhttps://abs.twimg.com/emoji/v2/... draggable="false" alt="☑️" title="Kästchen mit Häkchen" aria-label="Emoji: Kästchen mit Häkchen">gender identity9/9Loved working on this with colleagues @JRaney_MD @Riagpal @KimHoangMD @MikeGisondi">


