1/
Ready for a #NeoNeph #tweetorial? Let& #39;s look at kidney support therapy (KST) in #neonates.
@ASPNeph @EBNEO @MedTweetorials @MedEdBot @IrishNeonatal @AAPneonatal #SoMe
Credit: NICKS course by @DDD_Askenazi & team. Great article by @menonshina https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6777586/">https://www.ncbi.nlm.nih.gov/pmc/artic...
Ready for a #NeoNeph #tweetorial? Let& #39;s look at kidney support therapy (KST) in #neonates.
@ASPNeph @EBNEO @MedTweetorials @MedEdBot @IrishNeonatal @AAPneonatal #SoMe
Credit: NICKS course by @DDD_Askenazi & team. Great article by @menonshina https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6777586/">https://www.ncbi.nlm.nih.gov/pmc/artic...
2/
First, what are the indications for KST?
The classic AEIOU + to allow optimization of nutrition which is critical in the neonatal population.
First, what are the indications for KST?
The classic AEIOU + to allow optimization of nutrition which is critical in the neonatal population.
3/
Before initiation of KST, a multidisciplinary discussion between neo and neph needs to happen and include the family when assessing candidacy for KST. Often, pulmonary status is a major determinant of the yield of KST in neonates esp in babies with pulmonary hypoplasia.
Before initiation of KST, a multidisciplinary discussion between neo and neph needs to happen and include the family when assessing candidacy for KST. Often, pulmonary status is a major determinant of the yield of KST in neonates esp in babies with pulmonary hypoplasia.
4/ What are the necessary steps before initiation of KST?
A. Ensure adequate MAP/GA for perfusion
B. Replace nephrotoxic medications
C. Evaluate infant for abdominal compartment syndrome, why? could affect kidney perfusion
D. Diuretic +/- albumin trial, not for too long though.
A. Ensure adequate MAP/GA for perfusion
B. Replace nephrotoxic medications
C. Evaluate infant for abdominal compartment syndrome, why? could affect kidney perfusion
D. Diuretic +/- albumin trial, not for too long though.
5/ What are the principals of KST?
A. Clearance (diffusive, osmotic or convective)
B. Fluid removal (osmotic or convective)
Life examples: tea bag in a cup of water (diffusion), coffee machine, waterfalls (convection).
For all modalities, you need blood flowing and a filter.
A. Clearance (diffusive, osmotic or convective)
B. Fluid removal (osmotic or convective)
Life examples: tea bag in a cup of water (diffusion), coffee machine, waterfalls (convection).
For all modalities, you need blood flowing and a filter.
6/ Options for KST for neonates and infants < 1.5-2 Kg are sometimes limited.
For babies without significant abdominal malformations, PD is a good choice.
A. Acute PD catheters could be some nephrologists at the bedside to provide manual PD. Main risk is leakage.
For babies without significant abdominal malformations, PD is a good choice.
A. Acute PD catheters could be some nephrologists at the bedside to provide manual PD. Main risk is leakage.
7/
B. Surgical PD catheter: better than A, however patient weight & abdominal conditions (wall defects, CDH) could be barriers. Leakage, esp if used immediately is a painful limitation
Mechanisms of PD include diffusion/osmosis (your tea cup example), negligible convection.
B. Surgical PD catheter: better than A, however patient weight & abdominal conditions (wall defects, CDH) could be barriers. Leakage, esp if used immediately is a painful limitation
Mechanisms of PD include diffusion/osmosis (your tea cup example), negligible convection.
8/
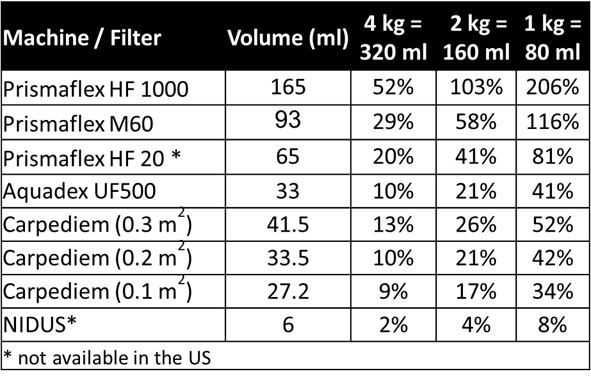
Hemodialysis & CRRT are challenging in neonates in the absence of small-volume extracorporeal circuits. Advanced-neonatal care centers use devices as aquadex & carpediem which have smaller volumes. See below for comparison of available machines.
Hemodialysis & CRRT are challenging in neonates in the absence of small-volume extracorporeal circuits. Advanced-neonatal care centers use devices as aquadex & carpediem which have smaller volumes. See below for comparison of available machines.
9/
Some of the above devices are available in the US
Can you think of one condition when it is life-saving to perform urgent HD in a neonate to achieve rapid clearance?
In that condition, there& #39;re case reports of using high-dose CRRT as well. Let me know your answer https://abs.twimg.com/emoji/v2/... draggable="false" alt="😉" title="Zwinkerndes Gesicht" aria-label="Emoji: Zwinkerndes Gesicht">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="😉" title="Zwinkerndes Gesicht" aria-label="Emoji: Zwinkerndes Gesicht">
Some of the above devices are available in the US
Can you think of one condition when it is life-saving to perform urgent HD in a neonate to achieve rapid clearance?
In that condition, there& #39;re case reports of using high-dose CRRT as well. Let me know your answer
10/
The prismaflex (volume of 100-165 ml) could easily be used in babies on ECMO since the extracorporeal volume and anticoagulation are already taken care of https://abs.twimg.com/emoji/v2/... draggable="false" alt="🙂" title="Leicht lächelndes Gesicht" aria-label="Emoji: Leicht lächelndes Gesicht">. When using the prismaflex you will have the options to run CVVH, CVVHD or CVVHDF.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🙂" title="Leicht lächelndes Gesicht" aria-label="Emoji: Leicht lächelndes Gesicht">. When using the prismaflex you will have the options to run CVVH, CVVHD or CVVHDF.
The prismaflex (volume of 100-165 ml) could easily be used in babies on ECMO since the extracorporeal volume and anticoagulation are already taken care of
11/
Aquapheresis (ultrafiltration/SCUF) & modified aquapheresis (CVVH) been used in adults with CHF, and several pediatric centers are currently using it as a modality for KST in neonates. At @NCHforDocs, these modalities will soon be available as options for neonatal KST.
Aquapheresis (ultrafiltration/SCUF) & modified aquapheresis (CVVH) been used in adults with CHF, and several pediatric centers are currently using it as a modality for KST in neonates. At @NCHforDocs, these modalities will soon be available as options for neonatal KST.
12/
We will discuss aquapheresis & our experience (with our aqua lead @BethAVogtMD1) in a separate #tweetorial.
I hope you enjoyed this brief summary. Let me know if there& #39;s a particular part that you wish to learn more about https://abs.twimg.com/emoji/v2/... draggable="false" alt="🙂" title="Leicht lächelndes Gesicht" aria-label="Emoji: Leicht lächelndes Gesicht">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🙂" title="Leicht lächelndes Gesicht" aria-label="Emoji: Leicht lächelndes Gesicht">
Thank you for reading.
We will discuss aquapheresis & our experience (with our aqua lead @BethAVogtMD1) in a separate #tweetorial.
I hope you enjoyed this brief summary. Let me know if there& #39;s a particular part that you wish to learn more about
Thank you for reading.

 Read on Twitter
Read on Twitter