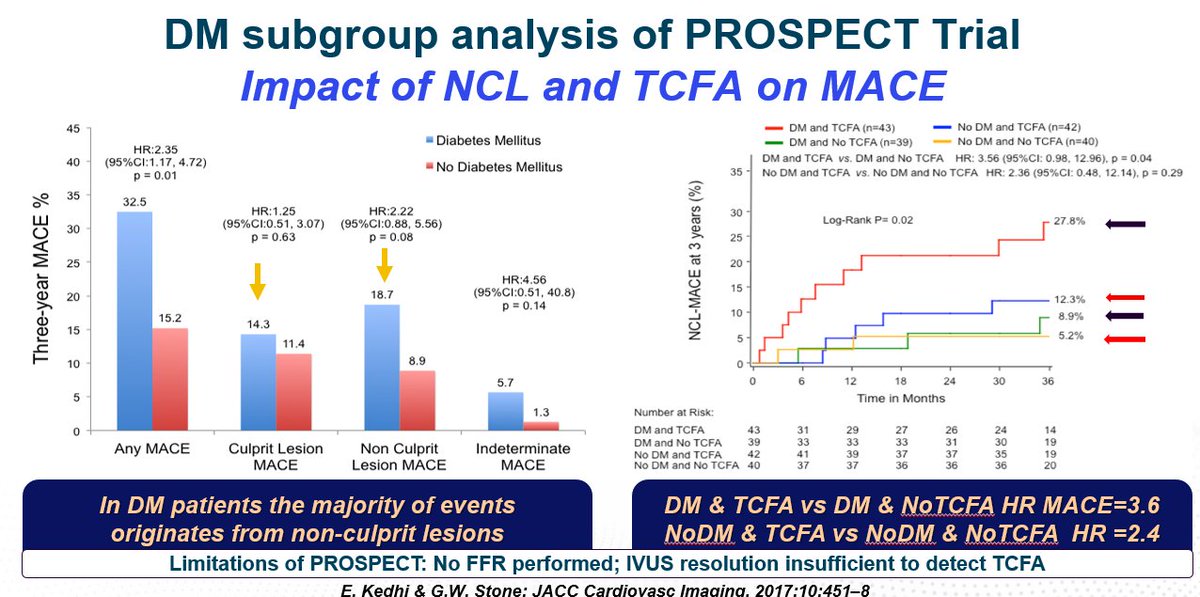
1/ COMBINE (OCT–FFR): Using OCT in DM to detect risk
FFR negative lesions, according to contemporary trial data, are very low risk for subsequent events. BUT...DM patients are a unique entity. What if we could use OCT, with its incredible resolution, to identify high risk - TCFA.
FFR negative lesions, according to contemporary trial data, are very low risk for subsequent events. BUT...DM patients are a unique entity. What if we could use OCT, with its incredible resolution, to identify high risk - TCFA.
3/ COMBINE -
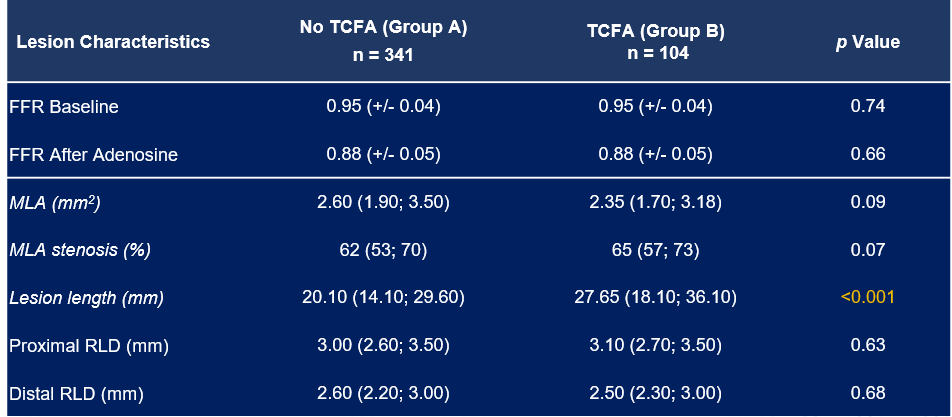
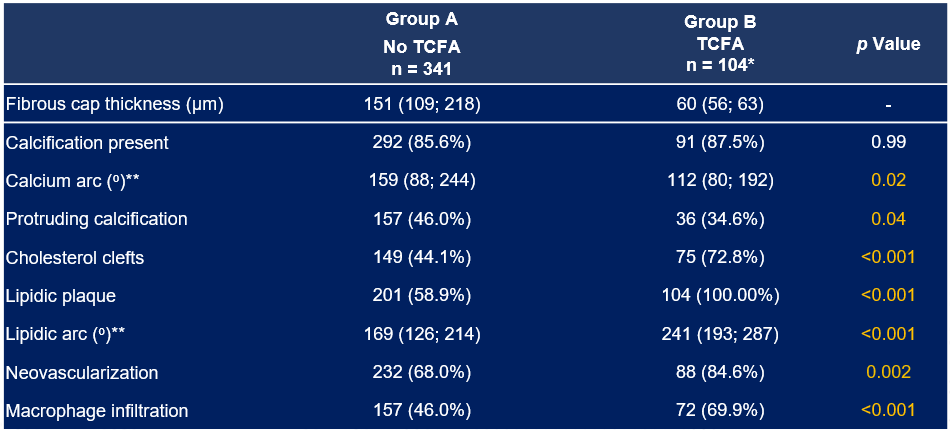
intermediate stenosis DS ≥ 40% and ≤ 80%,
FFR + - revasc ==> follow
FFR - TCFA + ==> follow
FFR - TCFA - ==> follow
intermediate stenosis DS ≥ 40% and ≤ 80%,
FFR + - revasc ==> follow
FFR - TCFA + ==> follow
FFR - TCFA - ==> follow
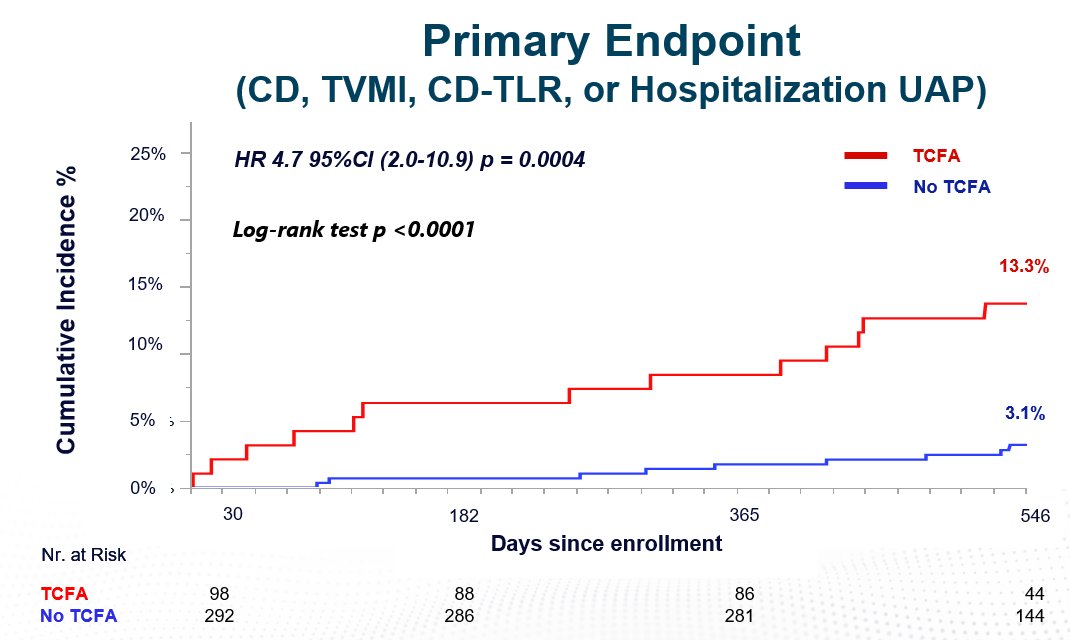
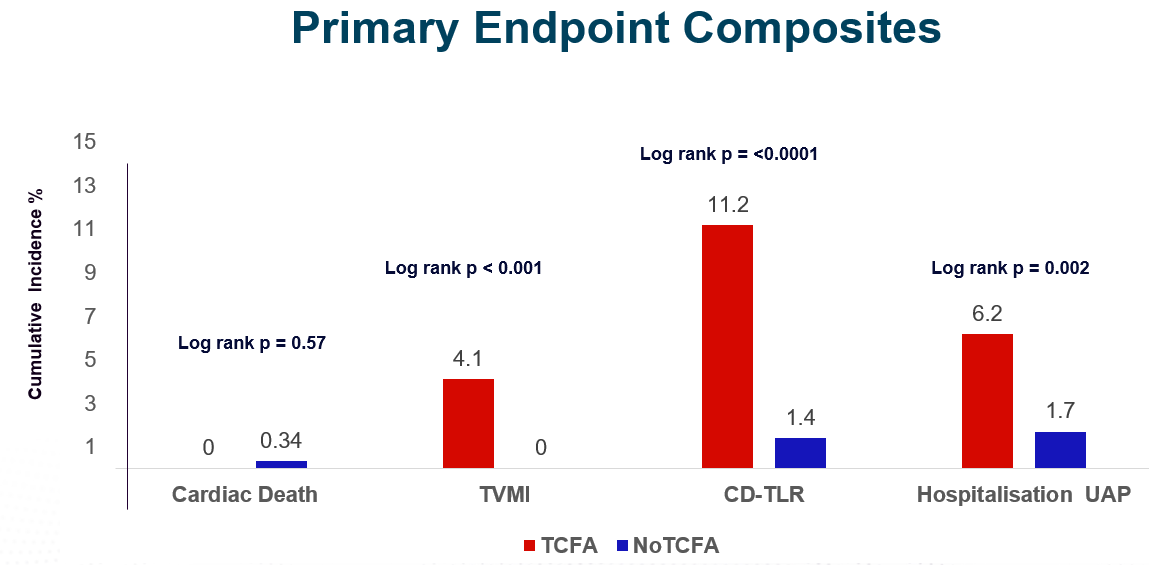
4/ Primary endpoint: The incidence of target lesion MACE: Cardiac death
target vessel myocardial infarction (MI)
clinically-driven target lesion revascularisation (TLR) hospitalisation due to unstable or progressive angina
at 18 months
target vessel myocardial infarction (MI)
clinically-driven target lesion revascularisation (TLR) hospitalisation due to unstable or progressive angina
at 18 months
10/ So..
- Even in FFR - patients, TCFA is bad.
- TCFA may lead to more events by TV-MI, UA, TLR
So know there is data to suggest that there is VP, even when FFR is -
Imagine if the OCT catheter could predict the FFR
#FUSION #VFR @DrAllenJ @ESHLOF @MaeharaAkiko @zhenzhang99
- Even in FFR - patients, TCFA is bad.
- TCFA may lead to more events by TV-MI, UA, TLR
So know there is data to suggest that there is VP, even when FFR is -
Imagine if the OCT catheter could predict the FFR
#FUSION #VFR @DrAllenJ @ESHLOF @MaeharaAkiko @zhenzhang99

 Read on Twitter
Read on Twitter