1/
How does a city& #39;s trauma system come together to both prepare for the expected surge of the #COVIDー19 #pandemic & manage the ongoing #epidemic of #gunviolence & other trauma?
Through a great collaborative effort, we published the #Philadelphia experience in @JTraumAcuteSurg
How does a city& #39;s trauma system come together to both prepare for the expected surge of the #COVIDー19 #pandemic & manage the ongoing #epidemic of #gunviolence & other trauma?
Through a great collaborative effort, we published the #Philadelphia experience in @JTraumAcuteSurg
2/
The full paper is published ahead of print here: https://journals.lww.com/jtrauma/Citation/9000/Trauma_center_activity_and_surge_response_during.97821.aspx
It">https://journals.lww.com/jtrauma/C... represents the importance of #teamwork in ensuring a robust, rapid, coordinated effort to manage an evolving threat
The full paper is published ahead of print here: https://journals.lww.com/jtrauma/Citation/9000/Trauma_center_activity_and_surge_response_during.97821.aspx
It">https://journals.lww.com/jtrauma/C... represents the importance of #teamwork in ensuring a robust, rapid, coordinated effort to manage an evolving threat
3/
Our publication timing coincides with a brutal #July4th weekend where #Philadelphia saw over 30 people shot including several children
But how did the #pandemic and #socialdistancing mandate affect trauma volume in our centers?
Our publication timing coincides with a brutal #July4th weekend where #Philadelphia saw over 30 people shot including several children
But how did the #pandemic and #socialdistancing mandate affect trauma volume in our centers?
4/
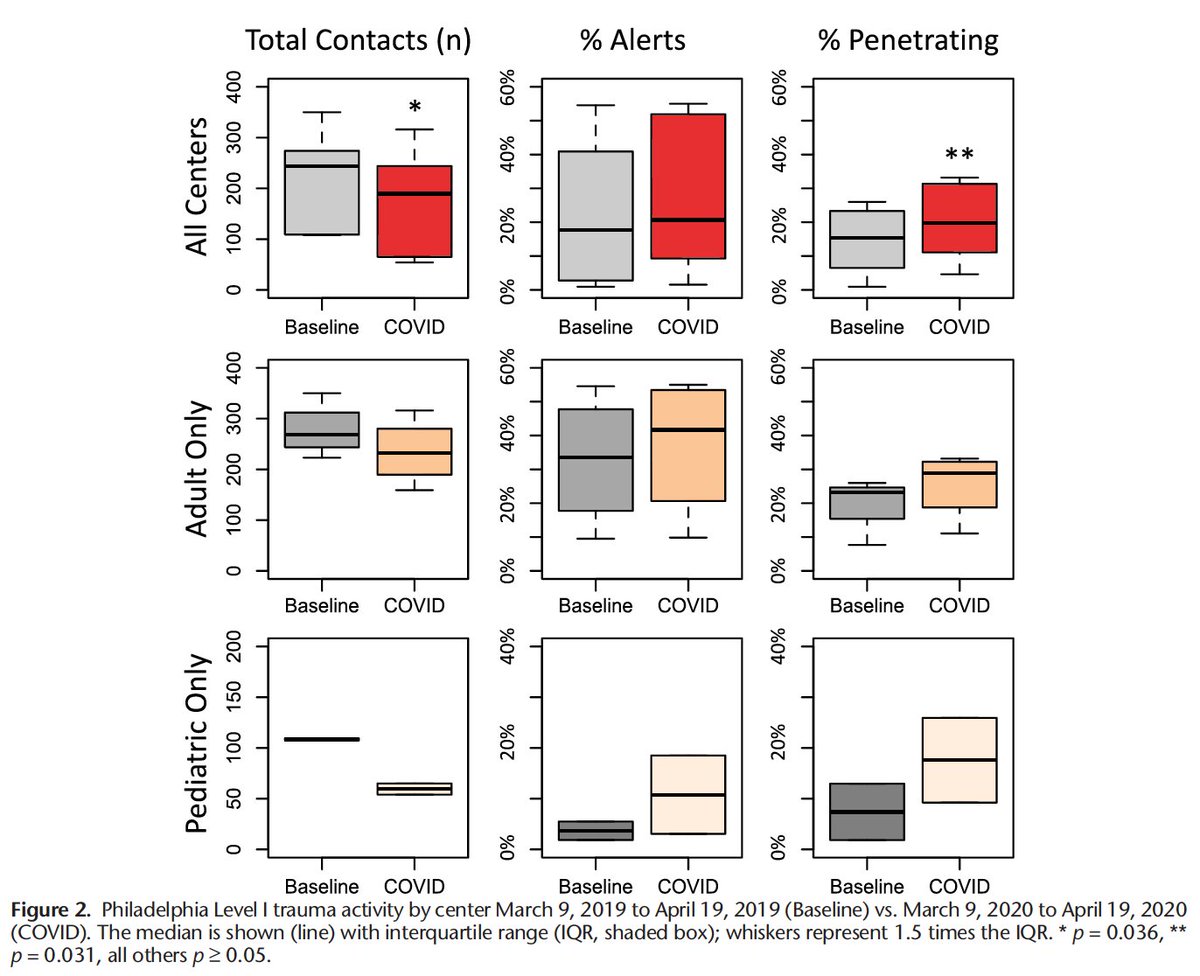
We found that, despite our overall #trauma volume being lower than usual, the number and proportion of #penetrating trauma actually increased in the first several weeks of the #pandemic.
We found that, despite our overall #trauma volume being lower than usual, the number and proportion of #penetrating trauma actually increased in the first several weeks of the #pandemic.
5/
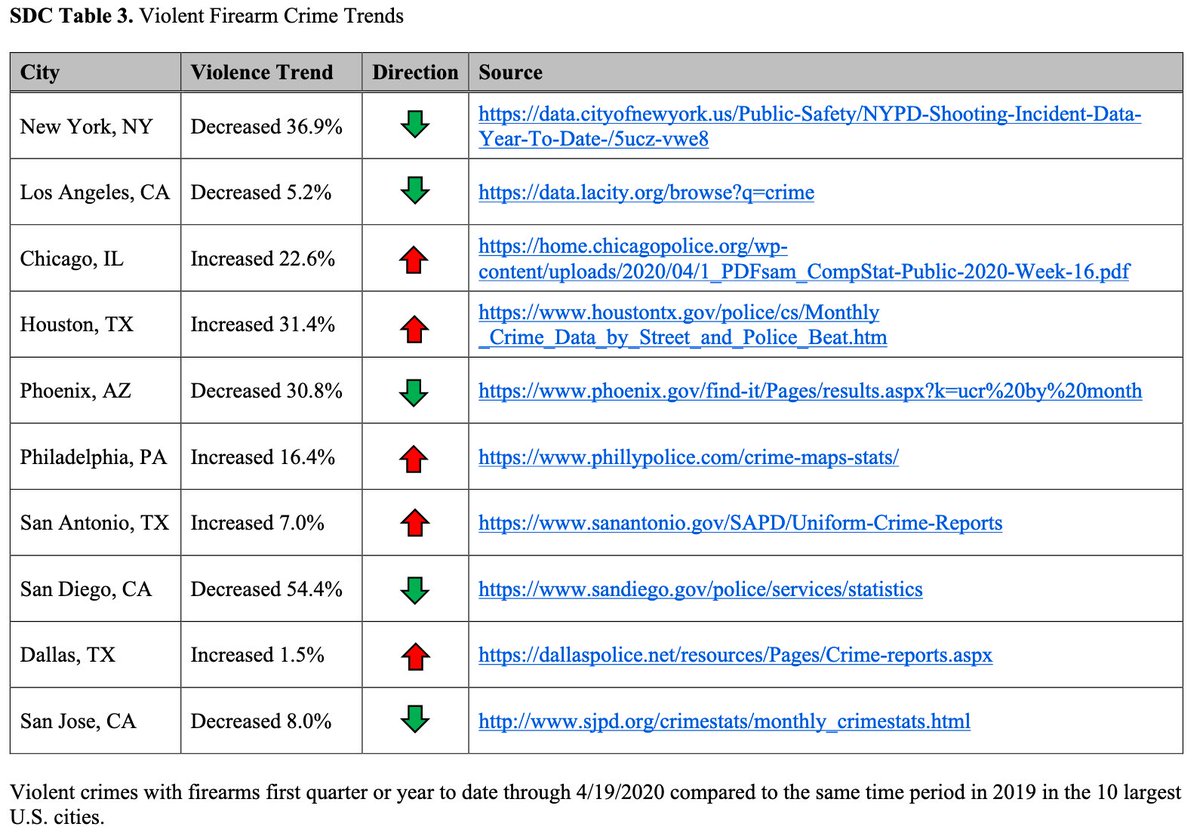
This trend was also seen in other cities including #Chicago, #Houston, #SanAntonio, and #Dallas
#gunviolence
This trend was also seen in other cities including #Chicago, #Houston, #SanAntonio, and #Dallas
#gunviolence
6/
Causes are likely multifactorial including:
-increased unstructured time
-increase in #gun sales
-higher unemployment/financial strain
But we have seen this #epidemic for a long time - as with many things, #COVID19 just brought it into sharper focus.
Causes are likely multifactorial including:
-increased unstructured time
-increase in #gun sales
-higher unemployment/financial strain
But we have seen this #epidemic for a long time - as with many things, #COVID19 just brought it into sharper focus.
7/
Through #geospatial mapping, we were able to find a significant relationship of shooting events occurring with a higher incidence in those #Philadelphia neighborhoods most affected by #COVID19 infection.
Through #geospatial mapping, we were able to find a significant relationship of shooting events occurring with a higher incidence in those #Philadelphia neighborhoods most affected by #COVID19 infection.
8/
An association b/w #race and both #COVID19 incidence and severity has been documented.
The #geospatial relationship identified in our study suggests the social determinants of health contributing to high viral concentration likely also correlate with endemic violence.
An association b/w #race and both #COVID19 incidence and severity has been documented.
The #geospatial relationship identified in our study suggests the social determinants of health contributing to high viral concentration likely also correlate with endemic violence.
9/
Many of the highest-density ZIP codes represent #Philadelphia neighborhoods that have suffered from poor socioeconomic conditions, & these feed into two of the adult and one pediatric #trauma centers that most accounted for the increased proportion of penetrating trauma
Many of the highest-density ZIP codes represent #Philadelphia neighborhoods that have suffered from poor socioeconomic conditions, & these feed into two of the adult and one pediatric #trauma centers that most accounted for the increased proportion of penetrating trauma
10/
Combined w/ the surge of #COVID19 patients requiring #criticalcare, this worsening of the #trauma #epidemic posed a significant threat to our city& #39;s ability to maintain trauma readiness, especially during the early dynamic phase of the #pandemic
How did we approach this?
Combined w/ the surge of #COVID19 patients requiring #criticalcare, this worsening of the #trauma #epidemic posed a significant threat to our city& #39;s ability to maintain trauma readiness, especially during the early dynamic phase of the #pandemic
How did we approach this?
11/
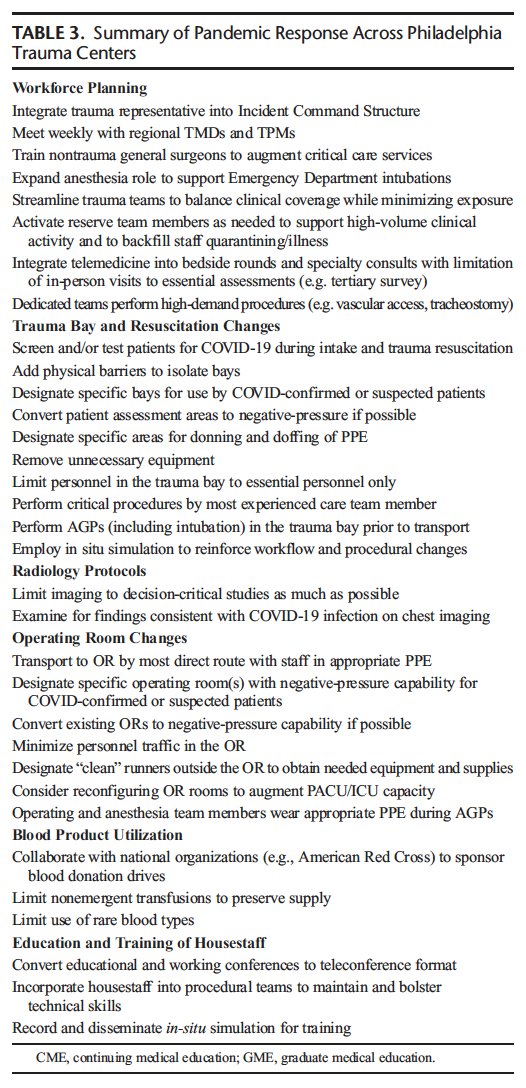
We individually adapted national guidance from @ACSTrauma ( https://www.facs.org/media/press-releases/2020/covid-trauma-031920)">https://www.facs.org/media/pre... but also felt it critical to work together across our trauma system.
So we set up a citywide weekly teleconference of trauma directors/managers-forming a regional medical operations center
We individually adapted national guidance from @ACSTrauma ( https://www.facs.org/media/press-releases/2020/covid-trauma-031920)">https://www.facs.org/media/pre... but also felt it critical to work together across our trauma system.
So we set up a citywide weekly teleconference of trauma directors/managers-forming a regional medical operations center
12/
This allowed - in addition to local preparations - the ability to share current #COVID19 & trauma patient census data, facility-level surge activities, #PPE postures, and clinical lessons learned from managing #pandemic patients, especially in its early dynamic phase
This allowed - in addition to local preparations - the ability to share current #COVID19 & trauma patient census data, facility-level surge activities, #PPE postures, and clinical lessons learned from managing #pandemic patients, especially in its early dynamic phase
13/
Some more specific benefits of our collaboration included augmenting adult center capacity through use of pediatric centers, modifications to trauma airway management & ventilator use, coordinating #PPE protocols across centers, and sharing of care #guidelines
Some more specific benefits of our collaboration included augmenting adult center capacity through use of pediatric centers, modifications to trauma airway management & ventilator use, coordinating #PPE protocols across centers, and sharing of care #guidelines
14/
The early #pandemic phase was dynamic, w/ rapidly evolving guidance and challenges.
Coordination to both face this threat & ensure ongoing readiness for other emergencies (including #trauma) is critical-siloed adoption could have delayed care & led to patient or staff harm.
The early #pandemic phase was dynamic, w/ rapidly evolving guidance and challenges.
Coordination to both face this threat & ensure ongoing readiness for other emergencies (including #trauma) is critical-siloed adoption could have delayed care & led to patient or staff harm.
15/
We hope that by sharing our experience we may help
other centers & regions prepare for future simultaneous surges in both critically ill & injured patients.
I want to thank my co-authors & the wider team at all our #Philadelphia centers that made this response possible
We hope that by sharing our experience we may help
other centers & regions prepare for future simultaneous surges in both critically ill & injured patients.
I want to thank my co-authors & the wider team at all our #Philadelphia centers that made this response possible

 Read on Twitter
Read on Twitter