What if 2m/6ft is not enough?
I& #39;m concerned our & #39;opening& #39; guidelines & restrictions may not be considering airborne microdroplet transmission of #SARSCoV2 #COVID19 sufficiently. What does that mean?
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🗨️" title="Left speech bubble" aria-label="Emoji: Left speech bubble">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🗨️" title="Left speech bubble" aria-label="Emoji: Left speech bubble"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="🦠" title="Microbe" aria-label="Emoji: Microbe">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🦠" title="Microbe" aria-label="Emoji: Microbe">
Let& #39;s talk. (Over a safe distance.)
1/23
I& #39;m concerned our & #39;opening& #39; guidelines & restrictions may not be considering airborne microdroplet transmission of #SARSCoV2 #COVID19 sufficiently. What does that mean?
Let& #39;s talk. (Over a safe distance.)
1/23
We& #39;ve seen a few studies now where groups of people in enclosed spaces with limited air circulation has led to outbreaks of infection.
Tracing exact contacts for the entire duration of the event is hard, but in most cases it seems unlikely all infected had direct contact.
2/23
Tracing exact contacts for the entire duration of the event is hard, but in most cases it seems unlikely all infected had direct contact.
2/23
To be clear from the start: I am *not* discounting other modes of transmission, like closer-contact droplets  https://abs.twimg.com/emoji/v2/... draggable="false" alt="💧" title="Droplet" aria-label="Emoji: Droplet"> & fomites
https://abs.twimg.com/emoji/v2/... draggable="false" alt="💧" title="Droplet" aria-label="Emoji: Droplet"> & fomites  https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚪" title="Door" aria-label="Emoji: Door"> (surface transmission). But I feel these are better understood & our strategies consider these heavily already.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚪" title="Door" aria-label="Emoji: Door"> (surface transmission). But I feel these are better understood & our strategies consider these heavily already.
This thread isn& #39;t for those.
3/23
This thread isn& #39;t for those.
3/23
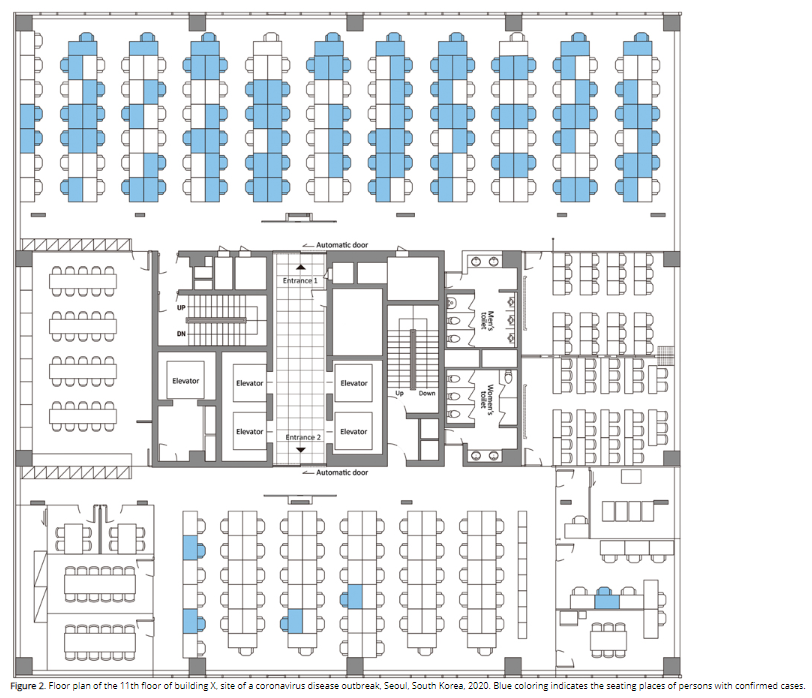
In a call centre in South Korea, 94/216 employees on a floor (notably - almost all on 1 side of that floor) became infected. The & #39;attack rate& #39; (proportion who got infected) was 44%.
https://wwwnc.cdc.gov/eid/article/26/8/20-1274_article
4/23">https://wwwnc.cdc.gov/eid/artic...
https://wwwnc.cdc.gov/eid/article/26/8/20-1274_article
4/23">https://wwwnc.cdc.gov/eid/artic...
All household contacts were also traced & tested, & interestingly, the & #39;secondary attack rate& #39; (number of those who got infected) was 16% - much lower. Even though we might expect direct contact & fomite (infection through surfaces) transmission to be higher in households.
5/23
5/23
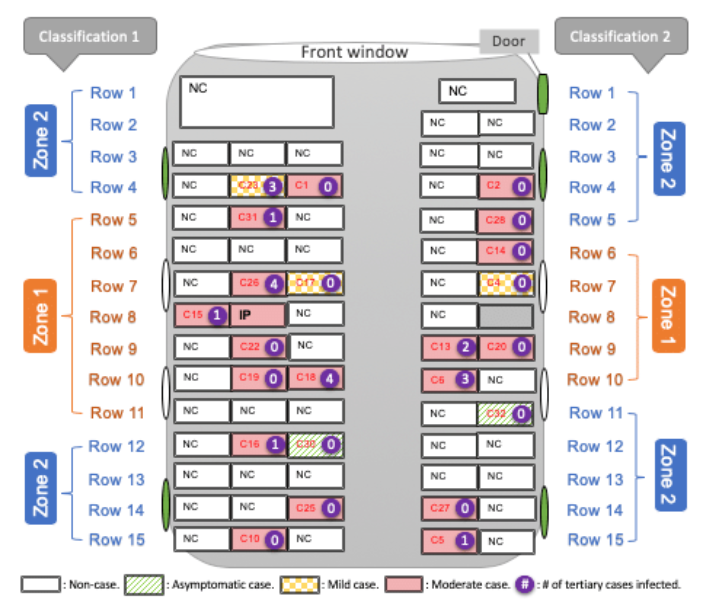
In another study, 2 busses went to an outdoor religious event (50 min ride each way). Bus #2 carried the index patient. Attendees mixed at the 150 min event & lunch, but took same bus (same seats) back.
299 ppl attended overall - 67 were on Bus #2
https://tinyurl.com/y7osnlxp
6/23">https://tinyurl.com/y7osnlxp&...
299 ppl attended overall - 67 were on Bus #2
https://tinyurl.com/y7osnlxp
6/23">https://tinyurl.com/y7osnlxp&...
30 ppl (excluding index) from the event were diagnosed with #COVID19 - 23 of these were ppl who rode on Bus2. 0 on Bus1, & 7 from the event who didn& #39;t arrive on busses (these reported close contact with index patient at event).
Bus was air conditioned & recirculating air.
7/23
Bus was air conditioned & recirculating air.
7/23
Here, index patient is marked & #39;IP& #39; (row 8). Though being near IP seems to have been risky, people throughout the bus, even quite far away, were infected. (Though many also were not!)
Attack rate on Bus2 was 34% vs 10% for overall event.
8/NN
Attack rate on Bus2 was 34% vs 10% for overall event.
8/NN
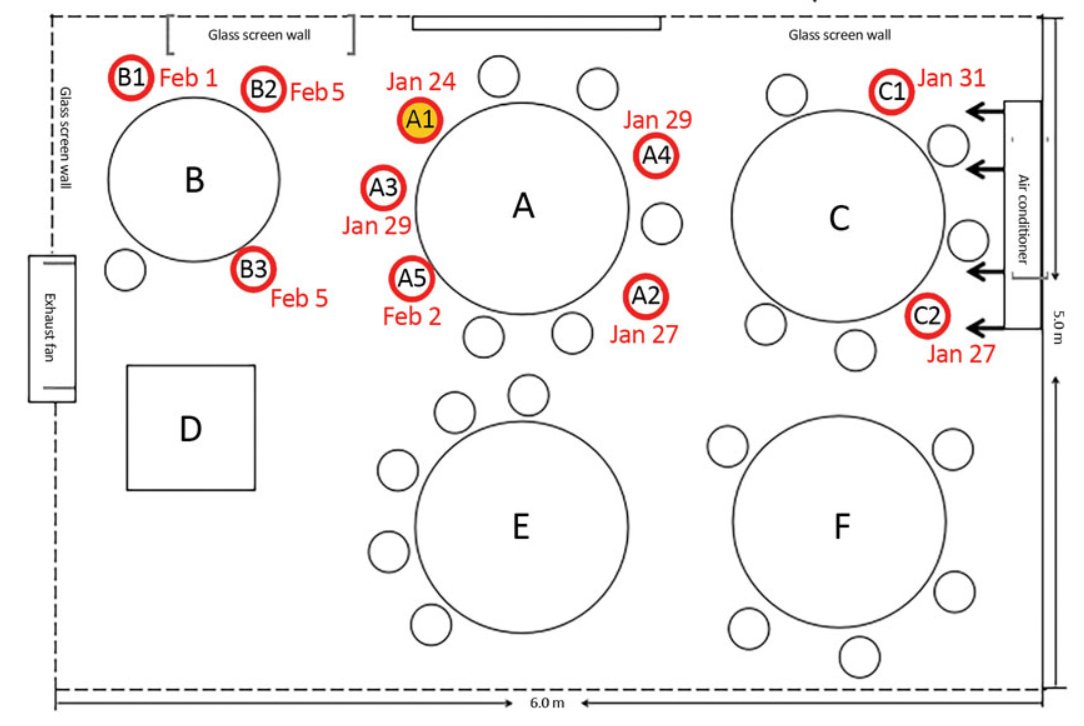
In a third study, 1 family (A) from Wuhan infected two other fams (B & C) in an air-conditioned, windowless restaurant. The families overlapped by 50-70 mins in seating.
83 ppl in total ate lunch that day on this floor, over 15 tables. Only 5 in families B & C were infected
9/23
83 ppl in total ate lunch that day on this floor, over 15 tables. Only 5 in families B & C were infected
9/23
So overall attack rate is low - 6%. But within flow of the air-con unit (excluding A), a considerable 45%.
A1 from family A developed symptoms 1st & is presumed to be index patient, but clearly infection of others in family A may not have been at restaurant.
10/23
A1 from family A developed symptoms 1st & is presumed to be index patient, but clearly infection of others in family A may not have been at restaurant.
10/23
In this study, distances were smaller, & possibility of spread from others in Family A seemingly can& #39;t be ruled out, but the lack of infections in other nearby families (D, E, F) who are not in air-con flow lines is notable.
11/23
11/23
Clearly, other forms of transmission are also important. However, these studies make me concerned that groups in closed spaces with limited air flow could be a risk for #COVID19 #SARSCoV2 transmission.
One that isn& #39;t covered by surface cleaning & 2m distance guidelines.
12/23
One that isn& #39;t covered by surface cleaning & 2m distance guidelines.
12/23
What do we know about airborne droplet spread?
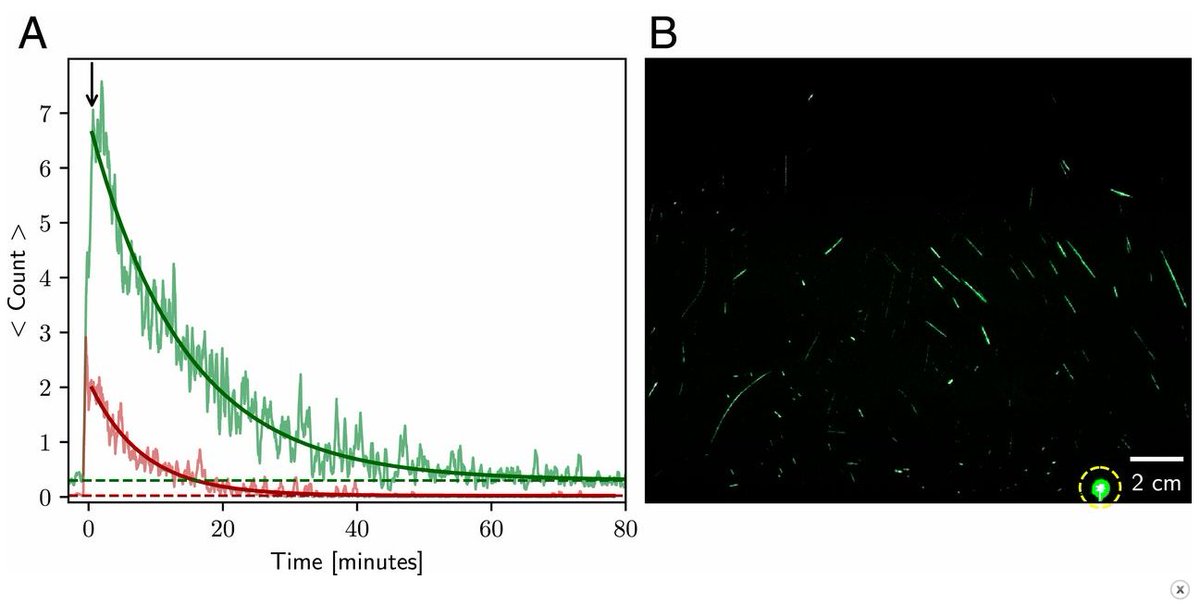
In speaking studies, smaller droplets (green) persist in air much longer than larger ones (red). These droplets could circulate considerably further than larger ones, which drop out of the air sooner.
https://www.pnas.org/content/early/2020/05/12/2006874117
13/23">https://www.pnas.org/content/e...
In speaking studies, smaller droplets (green) persist in air much longer than larger ones (red). These droplets could circulate considerably further than larger ones, which drop out of the air sooner.
https://www.pnas.org/content/early/2020/05/12/2006874117
13/23">https://www.pnas.org/content/e...
Importantly, however, as well as remaining airborne & having ability to circulate, infection potential of droplets is dependant on dehydration, saliva viral load & more.
We don& #39;t yet understand how this all interplays to create a risk of infection by airborne droplets.
14/23
We don& #39;t yet understand how this all interplays to create a risk of infection by airborne droplets.
14/23
However, without understanding the science perfectly, I think we can still say this is a risk to be aware of.
My concern is that while a lot of attention is going towards keeping 2m apart https://abs.twimg.com/emoji/v2/... draggable="false" alt="↔️" title="Left right arrow" aria-label="Emoji: Left right arrow"> & wiping doorknobs
https://abs.twimg.com/emoji/v2/... draggable="false" alt="↔️" title="Left right arrow" aria-label="Emoji: Left right arrow"> & wiping doorknobs  https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚪" title="Door" aria-label="Emoji: Door"> & surfaces, little is focused on people in enclosed spaces.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚪" title="Door" aria-label="Emoji: Door"> & surfaces, little is focused on people in enclosed spaces.
15/23
My concern is that while a lot of attention is going towards keeping 2m apart
15/23
Air circulation & filtration does seem to matter. The fact that we haven& #39;t seen large outbreaks linked to planes (even over longer flights) is interesting. Planes circulate & filter air frequently - so perhaps this can successfully prevent airborne transmission.  https://abs.twimg.com/emoji/v2/... draggable="false" alt="✈️" title="Airplane" aria-label="Emoji: Airplane">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="✈️" title="Airplane" aria-label="Emoji: Airplane"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="💧" title="Droplet" aria-label="Emoji: Droplet">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="💧" title="Droplet" aria-label="Emoji: Droplet"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">
16/23
16/23
Similarly, time likely matters. All of the above situations were >=50mins of exposure. Places like grocery stores, where trips are shorter & air flow likely aided by people coming & going (plus usual ventilation) are probably much lower risk.  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⏲️" title="Timer clock" aria-label="Emoji: Timer clock">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⏲️" title="Timer clock" aria-label="Emoji: Timer clock"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="💧" title="Droplet" aria-label="Emoji: Droplet">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="💧" title="Droplet" aria-label="Emoji: Droplet"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="🛒" title="Shopping cart" aria-label="Emoji: Shopping cart">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🛒" title="Shopping cart" aria-label="Emoji: Shopping cart">
17/23
17/23
What we remain unsure about are other forms of transport with less & #39;air attention& #39;: trains  https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚅" title="High-speed train with bullet nose" aria-label="Emoji: High-speed train with bullet nose">, busses
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚅" title="High-speed train with bullet nose" aria-label="Emoji: High-speed train with bullet nose">, busses  https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚍" title="Oncoming bus" aria-label="Emoji: Oncoming bus">, trams
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚍" title="Oncoming bus" aria-label="Emoji: Oncoming bus">, trams  https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚋" title="Tram car" aria-label="Emoji: Tram car">.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🚋" title="Tram car" aria-label="Emoji: Tram car">.
And busy, longer-visit enclosed spaces: restaurants https://abs.twimg.com/emoji/v2/... draggable="false" alt="🍽️" title="Fork and knife with plate" aria-label="Emoji: Fork and knife with plate">, offices
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🍽️" title="Fork and knife with plate" aria-label="Emoji: Fork and knife with plate">, offices  https://abs.twimg.com/emoji/v2/... draggable="false" alt="💻" title="Personal computer" aria-label="Emoji: Personal computer">, gyms
https://abs.twimg.com/emoji/v2/... draggable="false" alt="💻" title="Personal computer" aria-label="Emoji: Personal computer">, gyms  https://abs.twimg.com/emoji/v2/... draggable="false" alt="🏋️🏻" title="Person lifting weights (light skin tone)" aria-label="Emoji: Person lifting weights (light skin tone)">, waiting areas
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🏋️🏻" title="Person lifting weights (light skin tone)" aria-label="Emoji: Person lifting weights (light skin tone)">, waiting areas  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⚕️" title="Staff of aesculapius" aria-label="Emoji: Staff of aesculapius">.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⚕️" title="Staff of aesculapius" aria-label="Emoji: Staff of aesculapius">.
18/23
And busy, longer-visit enclosed spaces: restaurants
18/23
What can we do to reduce airborne #COVID19 risk?
Advice is likely to differ while we& #39;re uncertain. But some things might help:
- Prioritise outdoor restaurant seating https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌞" title="Sun with face" aria-label="Emoji: Sun with face">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌞" title="Sun with face" aria-label="Emoji: Sun with face">
- Open windows as much as when possible https://abs.twimg.com/emoji/v2/... draggable="false" alt="🪟" title="Window" aria-label="Emoji: Window">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🪟" title="Window" aria-label="Emoji: Window">
- Mask-wearing https://abs.twimg.com/emoji/v2/... draggable="false" alt="😷" title="Face with medical mask" aria-label="Emoji: Face with medical mask">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="😷" title="Face with medical mask" aria-label="Emoji: Face with medical mask">
- Reduce overall inside capacity https://abs.twimg.com/emoji/v2/... draggable="false" alt="👩👩👧👦" title="Family (woman, woman, girl, boy)" aria-label="Emoji: Family (woman, woman, girl, boy)">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="👩👩👧👦" title="Family (woman, woman, girl, boy)" aria-label="Emoji: Family (woman, woman, girl, boy)">
19/23
Advice is likely to differ while we& #39;re uncertain. But some things might help:
- Prioritise outdoor restaurant seating
- Open windows as much as when possible
- Mask-wearing
- Reduce overall inside capacity
19/23
If concerns about airborne transmission bear out, changes to air circulation systems/flows/patterns & filter qualities may make places safer.
In the short term, advice on masks & doing all possible to aid air exchange with the outside may make a real difference.
20/23
In the short term, advice on masks & doing all possible to aid air exchange with the outside may make a real difference.
20/23
The fact that it feels like this is something less easy to tackle (not simply putting 2m lines on a floor, or sanitising table-tops) makes it harder to talk about, I think.
We don& #39;t want to have more to be worried about! https://abs.twimg.com/emoji/v2/... draggable="false" alt="😫" title="Tired face" aria-label="Emoji: Tired face">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="😫" title="Tired face" aria-label="Emoji: Tired face">
21/23
We don& #39;t want to have more to be worried about!
21/23
But wishing won& #39;t make a possible risk go away.  https://abs.twimg.com/emoji/v2/... draggable="false" alt="✨" title="Sparkles" aria-label="Emoji: Sparkles">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="✨" title="Sparkles" aria-label="Emoji: Sparkles"> https://abs.twimg.com/emoji/v2/... draggable="false" alt="🤞🏻" title="Crossed fingers (light skin tone)" aria-label="Emoji: Crossed fingers (light skin tone)">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🤞🏻" title="Crossed fingers (light skin tone)" aria-label="Emoji: Crossed fingers (light skin tone)">
Instead, we should empower our reopening strategies to take into consideration these possible risks, & let people take put into their calculations about where & when they go. So they can make informed decisions. https://abs.twimg.com/emoji/v2/... draggable="false" alt="🧮" title="Abacus" aria-label="Emoji: Abacus">
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🧮" title="Abacus" aria-label="Emoji: Abacus">
22/23
Instead, we should empower our reopening strategies to take into consideration these possible risks, & let people take put into their calculations about where & when they go. So they can make informed decisions.
22/23
 Read on Twitter
Read on Twitter https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">https://abs.twimg.com/emoji/v2/... draggable="false" alt="🦠" title="Microbe" aria-label="Emoji: Microbe">Let& #39;s talk. (Over a safe distance.)1/23" title="What if 2m/6ft is not enough? I& #39;m concerned our & #39;opening& #39; guidelines & restrictions may not be considering airborne microdroplet transmission of #SARSCoV2 #COVID19 sufficiently. What does that mean?https://abs.twimg.com/emoji/v2/... draggable="false" alt="🗨️" title="Left speech bubble" aria-label="Emoji: Left speech bubble">https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">https://abs.twimg.com/emoji/v2/... draggable="false" alt="🦠" title="Microbe" aria-label="Emoji: Microbe">Let& #39;s talk. (Over a safe distance.)1/23" class="img-responsive" style="max-width:100%;"/>
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">https://abs.twimg.com/emoji/v2/... draggable="false" alt="🦠" title="Microbe" aria-label="Emoji: Microbe">Let& #39;s talk. (Over a safe distance.)1/23" title="What if 2m/6ft is not enough? I& #39;m concerned our & #39;opening& #39; guidelines & restrictions may not be considering airborne microdroplet transmission of #SARSCoV2 #COVID19 sufficiently. What does that mean?https://abs.twimg.com/emoji/v2/... draggable="false" alt="🗨️" title="Left speech bubble" aria-label="Emoji: Left speech bubble">https://abs.twimg.com/emoji/v2/... draggable="false" alt="🌬️" title="Wind blowing face" aria-label="Emoji: Wind blowing face">https://abs.twimg.com/emoji/v2/... draggable="false" alt="🦠" title="Microbe" aria-label="Emoji: Microbe">Let& #39;s talk. (Over a safe distance.)1/23" class="img-responsive" style="max-width:100%;"/>