1/ There is more to serum protein electrophoresis (SPEP) than meets the eye. A SPEP is a rich exam, with a wealth of information, that has been relegated to the land of malignant hematology with advances in lab testing. Let& #39;s rediscover its richness through a few clinical cases.
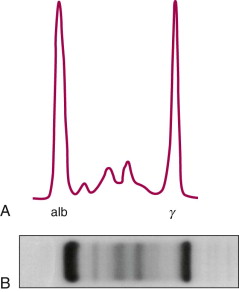
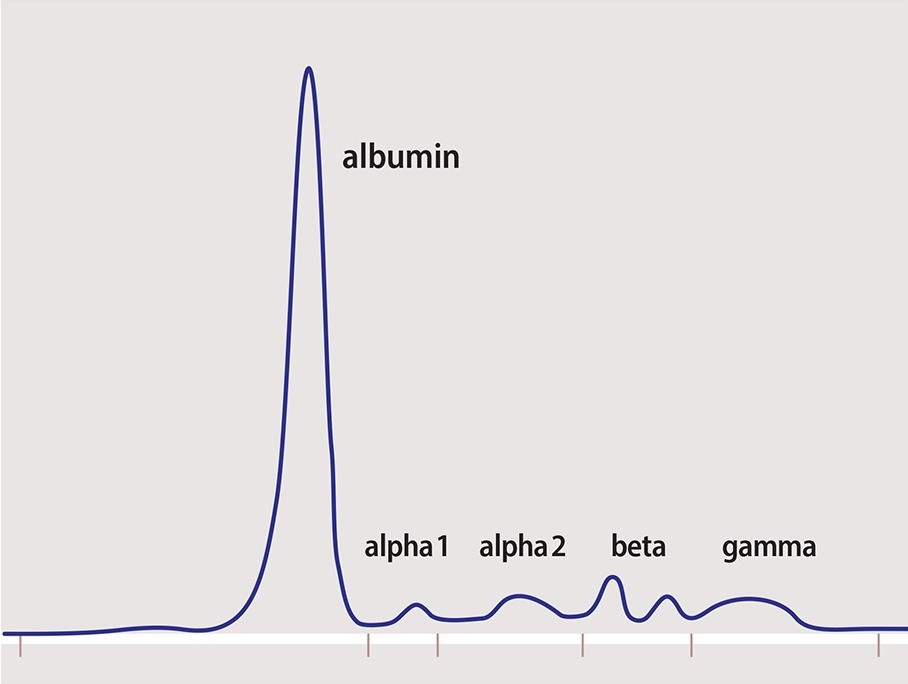
2/ This is what a normal SPEP pattern looks like. Albumin (60%) - globulins (40%). Normal A:G ratio 1.5-2.5.
Globulins comprise alpha 1, alpha 2, beta 1, beta 2 and gamma globulin portions.
Globulins comprise alpha 1, alpha 2, beta 1, beta 2 and gamma globulin portions.
3/ Alpha 1 portion: contains alpha1-antitrypsin. Positive acute phase reactant.  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">in AAT deficiency,
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">in AAT deficiency,  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">in inflammation & pregnancy.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">in inflammation & pregnancy.
Alpha 2 portion: contains ceruloplasmin & haptoglobin. Positive acute phase reactant.
Alpha 2 portion: contains ceruloplasmin & haptoglobin. Positive acute phase reactant.
4/ Beta 1 portion: contains transferrin. Pre-β region contains VLDL.
Beta 2 portion: contains beta-lipoprotein (mainly LDL).
IgA and IgM are in beta portion of SPEP.
Iron deficiency anemia causes https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow"> in transferrin and β1. Familial hypercholesterolemia causes a β2 spike.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow"> in transferrin and β1. Familial hypercholesterolemia causes a β2 spike.
Beta 2 portion: contains beta-lipoprotein (mainly LDL).
IgA and IgM are in beta portion of SPEP.
Iron deficiency anemia causes
5/ Gamma portion: main utility of SPEP.
If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">, suspect humoral immune dysfunction w/ hypogammaglobulinemia.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">, suspect humoral immune dysfunction w/ hypogammaglobulinemia.
If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">, suspect gammapathy and determine if monoclonal or polyclonal.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">, suspect gammapathy and determine if monoclonal or polyclonal.
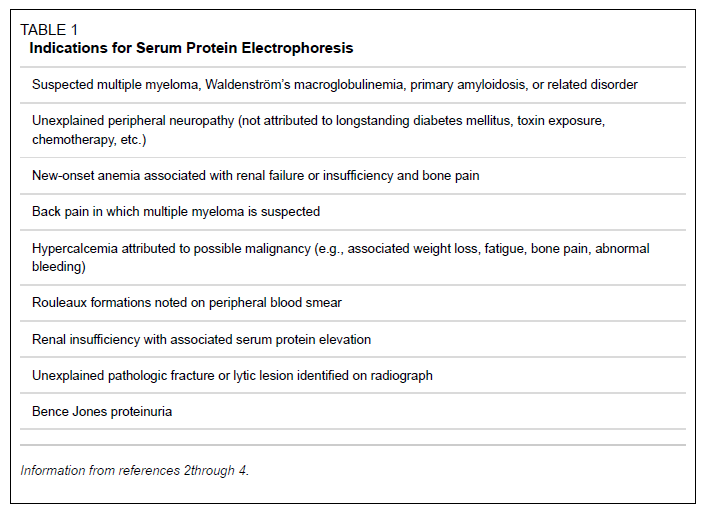
When to order a SPEP? (courtesy of AAFP, 2005)
If
If
When to order a SPEP? (courtesy of AAFP, 2005)
6/ What pathology is this pattern most compatible with?
7/ Answer: Inflammation
Note https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow"> albumin (
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow"> albumin ( https://abs.twimg.com/emoji/v2/... draggable="false" alt="➖" title="Heavy minus sign" aria-label="Emoji: Heavy minus sign">acute phase reactant) &
https://abs.twimg.com/emoji/v2/... draggable="false" alt="➖" title="Heavy minus sign" aria-label="Emoji: Heavy minus sign">acute phase reactant) &  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">α1/α2 (
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">α1/α2 ( https://abs.twimg.com/emoji/v2/... draggable="false" alt="➕" title="Heavy plus sign" aria-label="Emoji: Heavy plus sign">phase reactants).
https://abs.twimg.com/emoji/v2/... draggable="false" alt="➕" title="Heavy plus sign" aria-label="Emoji: Heavy plus sign">phase reactants).
Dehydration expected to cause https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow"> albumin (hemoconcentration).
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow"> albumin (hemoconcentration).
CVID expected to cause flattening of γ portion.
AAT def. causes flattening of α1 (SPEP now replaced w/ serum AAT level).
Note
Dehydration expected to cause
CVID expected to cause flattening of γ portion.
AAT def. causes flattening of α1 (SPEP now replaced w/ serum AAT level).
8/ What pathology is this pattern most compatible with?
9/ Answer: Nephrotic syndrome.
Loss of small-size proteins in urine ( https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">albumin, Ig) with compensatory
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">albumin, Ig) with compensatory  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">liver production of large proteins leading to α2 spike (α2-Macroglobulin & VLDL).
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">liver production of large proteins leading to α2 spike (α2-Macroglobulin & VLDL).
IDA can cause a β1 spike.
Loss of small-size proteins in urine (
IDA can cause a β1 spike.
10/ What pathology is this pattern most compatible with?
11/ Answer: cirrhosis
Early cirrhosis: beta-gamma bridging (related to increase in IgA and transferrin production?). Fairly characteristic of cirrhosis.
Advanced cirrhosis: poor synthetic function. https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">albumin.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">albumin.
A:G ratio<1 ( https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">albumin,
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">albumin,  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">Ig).
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">Ig).
Early cirrhosis: beta-gamma bridging (related to increase in IgA and transferrin production?). Fairly characteristic of cirrhosis.
Advanced cirrhosis: poor synthetic function.
A:G ratio<1 (
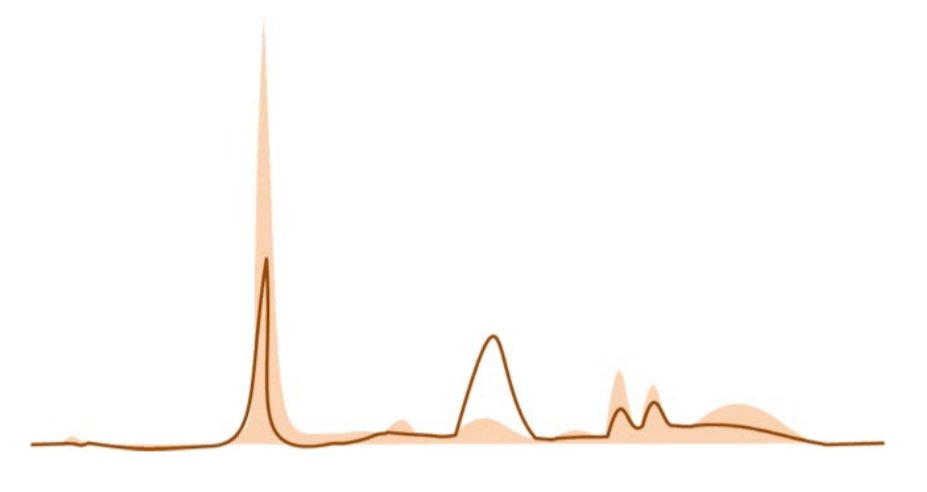
12/ What combination of pathologies is this pattern compatible with?
13/ Answer: SLE/cirrhosis
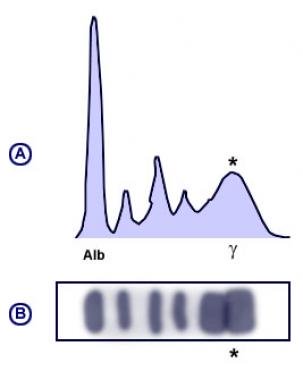
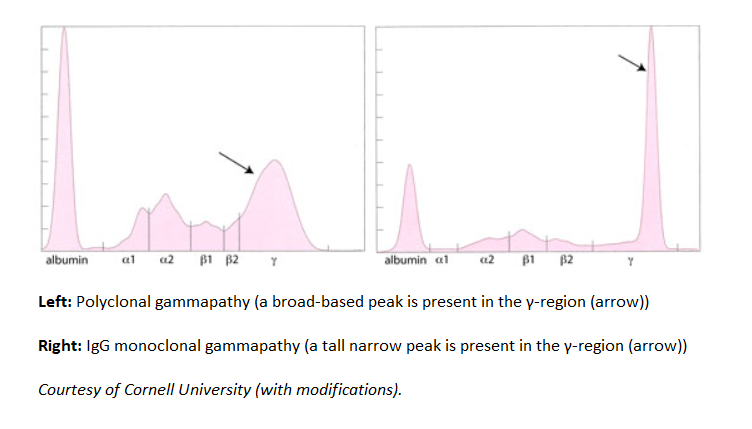
When faced with a gammapathy (large protein or gamma gap), identify if pattern is monoclonal or polyclonal.
When faced with a gammapathy (large protein or gamma gap), identify if pattern is monoclonal or polyclonal.
13/ Answer: SLE/cirrhosis
Broad-based peak in this case is suggestive of polyclonal gammapathy, a condition seen in both SLE and cirrhosis.
Broad-based peak in this case is suggestive of polyclonal gammapathy, a condition seen in both SLE and cirrhosis.
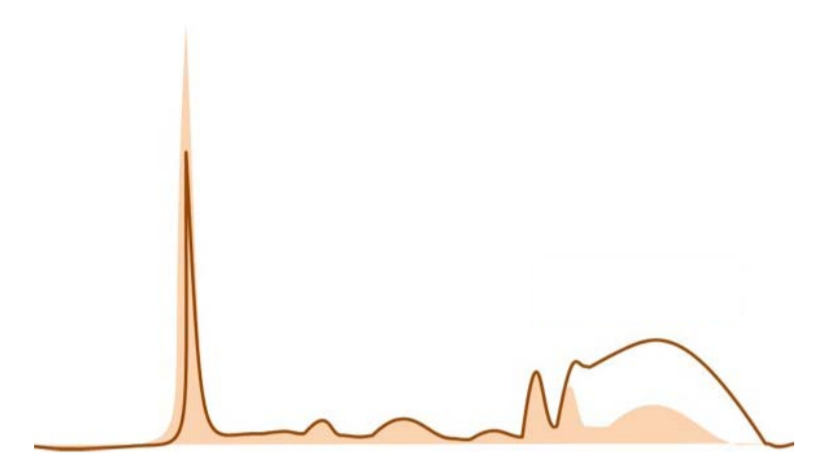
14/ What condition is the most likely diagnosis in this case?
15/ Answer: IgG multiple myeloma
There is evidence of monoclonal gammapathy (narrow-based peak). M-protein level seems elevated and predominant in the γ region, mostly compatible with smoldering or active IgG MM.
IgA MGUS should cause a smaller spike shifted more to the left.
There is evidence of monoclonal gammapathy (narrow-based peak). M-protein level seems elevated and predominant in the γ region, mostly compatible with smoldering or active IgG MM.
IgA MGUS should cause a smaller spike shifted more to the left.
16/ Always interpret SPEP in clinical context.
If a plasma cell disorder is still suspected despite a normal SPEP, order a serum free light chain assay (sFLC). Up to 20% of plasma dyscrasias only produce light chains lost in urine. A normal sFLC ratio is 0.26-1.65 ( https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow"> if GFR
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow"> if GFR  https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">).
https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">).
If a plasma cell disorder is still suspected despite a normal SPEP, order a serum free light chain assay (sFLC). Up to 20% of plasma dyscrasias only produce light chains lost in urine. A normal sFLC ratio is 0.26-1.65 (
Please share your thoughts/questions below.
Further reading:
Understanding and Interpreting Serum Protein Electrophoresis
https://www.aafp.org/afp/2005/0101/p105.html
https://www.aafp.org/afp/2005/... href=" https://www.sciencedirect.com/topics/medicine-and-dentistry/protein-electrophoresis
Interprétation">https://www.sciencedirect.com/topics/me... de l’électrophorèse
des protéines sériques. (in French)
http://www.fmc-tourcoing.org/new/wp-content/uploads/2015/12/Electrophores-des-proteines-seriques-R.pdf
Interesting">https://www.fmc-tourcoing.org/new/wp-co... cases:
http://ucsdlabmed.wikidot.com/chapter-7-laboratory-diagnosis-of-protein-abnormalities">https://ucsdlabmed.wikidot.com/chapter-7...
Understanding and Interpreting Serum Protein Electrophoresis
https://www.aafp.org/afp/2005/0101/p105.html
Interprétation">https://www.sciencedirect.com/topics/me... de l’électrophorèse
des protéines sériques. (in French)
http://www.fmc-tourcoing.org/new/wp-content/uploads/2015/12/Electrophores-des-proteines-seriques-R.pdf
Interesting">https://www.fmc-tourcoing.org/new/wp-co... cases:
http://ucsdlabmed.wikidot.com/chapter-7-laboratory-diagnosis-of-protein-abnormalities">https://ucsdlabmed.wikidot.com/chapter-7...

 Read on Twitter
Read on Twitter
 , suspect humoral immune dysfunction w/ hypogammaglobulinemia. If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">, suspect gammapathy and determine if monoclonal or polyclonal.When to order a SPEP? (courtesy of AAFP, 2005)" title="5/ Gamma portion: main utility of SPEP. If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">, suspect humoral immune dysfunction w/ hypogammaglobulinemia. If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">, suspect gammapathy and determine if monoclonal or polyclonal.When to order a SPEP? (courtesy of AAFP, 2005)" class="img-responsive" style="max-width:100%;"/>
, suspect humoral immune dysfunction w/ hypogammaglobulinemia. If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">, suspect gammapathy and determine if monoclonal or polyclonal.When to order a SPEP? (courtesy of AAFP, 2005)" title="5/ Gamma portion: main utility of SPEP. If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬇️" title="Downwards arrow" aria-label="Emoji: Downwards arrow">, suspect humoral immune dysfunction w/ hypogammaglobulinemia. If https://abs.twimg.com/emoji/v2/... draggable="false" alt="⬆️" title="Upwards arrow" aria-label="Emoji: Upwards arrow">, suspect gammapathy and determine if monoclonal or polyclonal.When to order a SPEP? (courtesy of AAFP, 2005)" class="img-responsive" style="max-width:100%;"/>