1/
Curious about the links between #overweight, #obesity, and #COVIDー19?
Let’s go one layer deeper than the headlines.
Here is a summary of the data so far reported in accepted manuscripts and pre-prints from large academic medical centers.
Curious about the links between #overweight, #obesity, and #COVIDー19?
Let’s go one layer deeper than the headlines.
Here is a summary of the data so far reported in accepted manuscripts and pre-prints from large academic medical centers.
2/
Cai et al. studied 383 COVID-19 patients admitted to Third People’s Hospital in Shenzen https://abs.twimg.com/emoji/v2/... draggable="false" alt="🇨🇳" title="Flag of China" aria-label="Emoji: Flag of China">.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🇨🇳" title="Flag of China" aria-label="Emoji: Flag of China">.
At baseline, 32% were overweight and 10.7% were obese.
Obese patients had 2.42-fold higher odds of developing severe pneumonia.
Cai et al. studied 383 COVID-19 patients admitted to Third People’s Hospital in Shenzen
At baseline, 32% were overweight and 10.7% were obese.
Obese patients had 2.42-fold higher odds of developing severe pneumonia.
3/
Interestingly, the data indicate that obese men were particularly susceptible to developing severe pneumonia.
They had an odds ratio of 5.70!
Interestingly, the data indicate that obese men were particularly susceptible to developing severe pneumonia.
They had an odds ratio of 5.70!
4/
Notes:
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">In East Asia overweight is BMI > 24 and obesity is BMI > 28, compared to cut-offs of 25 and 30 elsewhere.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">In East Asia overweight is BMI > 24 and obesity is BMI > 28, compared to cut-offs of 25 and 30 elsewhere.
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">The multivariate model was adjusted for history of including hypertension and diabetes
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">The multivariate model was adjusted for history of including hypertension and diabetes
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Retrospective design at a single center with no historical controls
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Retrospective design at a single center with no historical controls
Notes:
5/
Here is the pre-print submitted to The Lancet Infectious Diseases:
https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3556658">https://papers.ssrn.com/sol3/pape...
Here is the pre-print submitted to The Lancet Infectious Diseases:
https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3556658">https://papers.ssrn.com/sol3/pape...
6/
Simonnet et al. studied 124 consecutive patients admitted for ICU care at @CHU_Lille.
These patients were also compared to a historical control group of 306 patients admitted to the ICU for severe acute respiratory disease earlier in 2019.
Simonnet et al. studied 124 consecutive patients admitted for ICU care at @CHU_Lille.
These patients were also compared to a historical control group of 306 patients admitted to the ICU for severe acute respiratory disease earlier in 2019.
7/
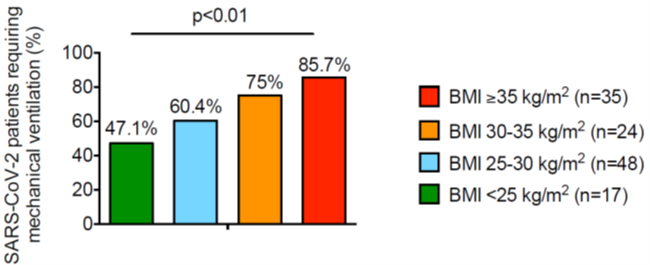
At baseline, 48% had BMI > 30 and 28% had BMI > 35.
86% of patients with BMI > 35 required invasive mechanical ventilation (IMV).
At baseline, 48% had BMI > 30 and 28% had BMI > 35.
86% of patients with BMI > 35 required invasive mechanical ventilation (IMV).
9/
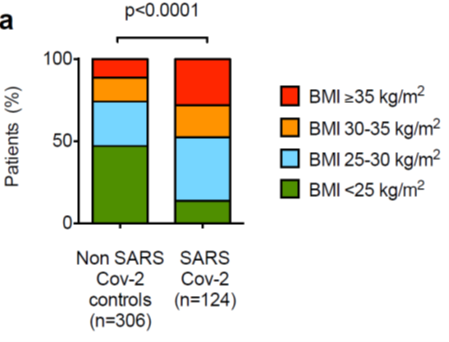
Interestingly, BMI distribution for SARS-CoV-2 patients was markedly different than in the historical cohort, skewing heavily toward higher BMI.
Interestingly, BMI distribution for SARS-CoV-2 patients was markedly different than in the historical cohort, skewing heavily toward higher BMI.
10/
Notes:
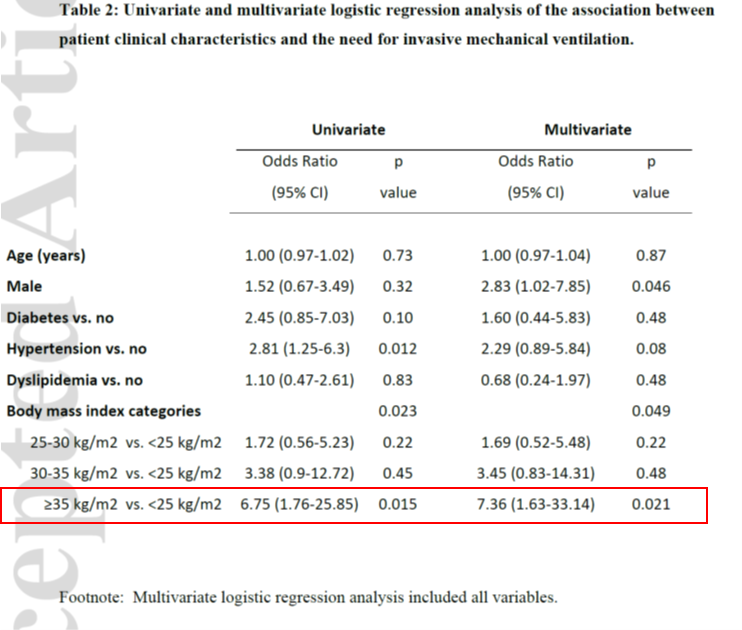
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Results remained significant in the multivariate model after adjusting for age, diabetes, and hypertension.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Results remained significant in the multivariate model after adjusting for age, diabetes, and hypertension.
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Retrospective design at a single center.
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Retrospective design at a single center.
Notes:
11/
Here is the accepted manuscript to appear in the official journal of the @ObesitySociety: https://onlinelibrary.wiley.com/doi/abs/10.1002/oby.22831">https://onlinelibrary.wiley.com/doi/abs/1...
Here is the accepted manuscript to appear in the official journal of the @ObesitySociety: https://onlinelibrary.wiley.com/doi/abs/10.1002/oby.22831">https://onlinelibrary.wiley.com/doi/abs/1...
12/
Lighter et al. reports on 3,615 individuals who were PCR-positive for COVID-19 at @nyulangone.
At baseline, 21% had BMI 30-34 and 16% had BMI > 35.
431 (12%) were transferred or admitted to the ICU.
Lighter et al. reports on 3,615 individuals who were PCR-positive for COVID-19 at @nyulangone.
At baseline, 21% had BMI 30-34 and 16% had BMI > 35.
431 (12%) were transferred or admitted to the ICU.
13/
For those > 60 y/o, there was no correlation with BMI and ICU admission.
For those < 60 y/o, patients with BMI 30-34 were 1.8X more likely to be admitted to ICU.
Patients with BMI > 35 were 3.6X more likely!
For those > 60 y/o, there was no correlation with BMI and ICU admission.
For those < 60 y/o, patients with BMI 30-34 were 1.8X more likely to be admitted to ICU.
Patients with BMI > 35 were 3.6X more likely!
14/
Notes:
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Retrospective design with no historical controls
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Retrospective design with no historical controls
 https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Manuscript does not detail the criteria used to admit patients to acute care or ICU
https://abs.twimg.com/emoji/v2/... draggable="false" alt="🔹" title="Small blue diamond" aria-label="Emoji: Small blue diamond">Manuscript does not detail the criteria used to admit patients to acute care or ICU
Notes:
15/
Here is the accepted manuscript from Clinical Infectious Diseases: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa415/5818333">https://academic.oup.com/cid/advan...
Here is the accepted manuscript from Clinical Infectious Diseases: https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa415/5818333">https://academic.oup.com/cid/advan...
16/
Bottom line: #overweight and #obesity appear to be correlated to more severe manifestations of #COVIDー19 and ICU-level care. While younger individuals typically fare better from COVID-19, obesity may exacerbate the issue in this population.
Bottom line: #overweight and #obesity appear to be correlated to more severe manifestations of #COVIDー19 and ICU-level care. While younger individuals typically fare better from COVID-19, obesity may exacerbate the issue in this population.
17/
This underscores the importance of being mindful of weight while we are under quarantine and taking proactive steps to protect ourselves in the event of a #secondwave.
BMI and weight matter here and providers should be mindful of this as they start seeing patients again!
This underscores the importance of being mindful of weight while we are under quarantine and taking proactive steps to protect ourselves in the event of a #secondwave.
BMI and weight matter here and providers should be mindful of this as they start seeing patients again!

 Read on Twitter
Read on Twitter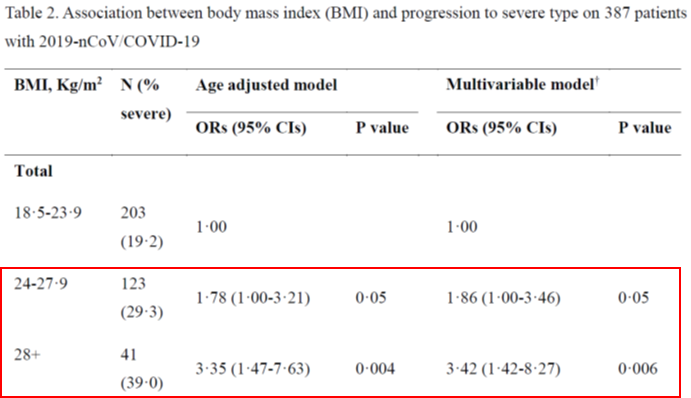 .At baseline, 32% were overweight and 10.7% were obese.Obese patients had 2.42-fold higher odds of developing severe pneumonia." title="2/Cai et al. studied 383 COVID-19 patients admitted to Third People’s Hospital in Shenzen https://abs.twimg.com/emoji/v2/... draggable="false" alt="🇨🇳" title="Flag of China" aria-label="Emoji: Flag of China">.At baseline, 32% were overweight and 10.7% were obese.Obese patients had 2.42-fold higher odds of developing severe pneumonia." class="img-responsive" style="max-width:100%;"/>
.At baseline, 32% were overweight and 10.7% were obese.Obese patients had 2.42-fold higher odds of developing severe pneumonia." title="2/Cai et al. studied 383 COVID-19 patients admitted to Third People’s Hospital in Shenzen https://abs.twimg.com/emoji/v2/... draggable="false" alt="🇨🇳" title="Flag of China" aria-label="Emoji: Flag of China">.At baseline, 32% were overweight and 10.7% were obese.Obese patients had 2.42-fold higher odds of developing severe pneumonia." class="img-responsive" style="max-width:100%;"/>